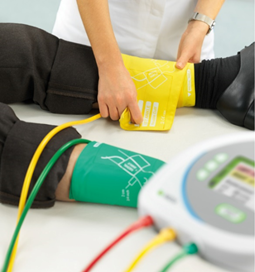
Preventive screening fod PAD on the basis of ABI measurement is recommended for individuals who are older, over or underweight and have family history of PAD.
There are many risk factors for Peripheral Arterial Disease (PAD) and some are non-modifiable and some are modifiable by a patient. And just as with any other disease, PAD patients are usually subject to both in a manner similar to individuals with other Cardio‑Vascular Diseases (CVDs).
The most common immutable risk factors for CVD are age, gender and family history (genetic predisposition), but all but a few patients are also subject to lifestyle-related factors such as obesity, smoking and physical inactivity. For example, with regards to Coronary Artery Disease (CAD), the most common type of CVD and the leading cause of mortality worldwide (of all CVDs and on its own), mortality increases between 2.3 and 2.7 times in males and 2.9 to 3.7 times in females for every decade of life (after the age of 50) [1, 2].
Family history also has an important role in CVD incidence, and it has been estimated that a parent with a history of premature atherosclerotic CVD increases an individual’s risk for CVD by a factor of 3 [3]. Unhealthy weight (being either overweight, obese or underweight) is another factor and one of considerable complexity as it is often invariably connected with other issues [4].
Why are Age, Weight and Family History a Critical Risk Factor for PAD?
Advanced age is positively correlated with an increased risk of PAD and the incidence of PAD increases with age – studies have shown that the risk of PAD increases approximately two to three times for every 10 year increase in age after the age of 40 [5].
This is strongly correlated in very old individuals as the incidence of PAD rises from 1 in 50 in the age group of individuals between 40 and 50 years old to 1 in 3 in groups composed of patients with ages ranging from 91 to 100 years [6].
Reasons for this are varied and range from generally recognised fact that atherosclerosis (the main mechanism for development of PAD) gets worse with age due to diminished physical activity (reduced muscle strength, balance, flexibility etc.) which has an antiatherogenic effect.
Research on the genetic basis of PAD is still in its infancy and studies have yet to identify definite genetic markers for PAD, while the more tangible and broad effects of family history are well established. Studies have shown that those with a family history of PAD are at twice the risk level of those individuals without a family history of PAD – this association was stronger for those younger than 68 and for individuals with more than one affected relative [7].
The association between weight (often expressed in as Body Mass Index or BMI) and PAD is more tentative in comparison with the other two aforementioned risk factors as it is often, when conducting studies on risk factors, difficult to distinguish the effects of high (or low) BMI and coexisting smoking, hypertension, dyslipidaemia and diabetes risk factors. Still, underweight individuals (those with a BMI less than 18.5 kg/m2) with PAD are at an increased risk of mortality, while older individuals with a greater BMI (but otherwise healthy) have a higher incidence of PAD [8, 9].
Preventive screening for PAD on the basis of ABI measurement is therefore recommended for individuals who are older (over 65), over or underweight (especially if subject to other risk factors for PAD specifically or CVDs in general) and have a family history of PAD [10].
References:
[1] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5491406/
[2] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3819990/
[3] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3319439/
[4] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5728753/
[5] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3281253/
[6] http://www.onlinejacc.org/content/accj/61/16/1736.full.pdf
[7] https://www.ahajournals.org/doi/full/10.1161/CIRCRESAHA.116.303518
[8] https://www.ncbi.nlm.nih.gov/pubmed/29088925
[9] https://academic.oup.com/aje/article/174/9/1036/168550
[10] https://www.ahajournals.org/doi/10.1161/CIR.0000000000000470
